These sensors, embedded in fabric, can monitor patients’ physical condition and alert healthcare workers before pressure sores form.
Hospital stays can be long and arduous; they can also cause serious complications. When a person lies in one position too long and begins to sweat, painful sores called pressure injuries (PIs) can form on the body, leading to infection or even death. A patient can develop a PI in a few days — or even a few hours. And once present, a PI is hard to treat.

Previously known as pressure ulcers, PIs affect 2.5 million patients and result in 60,000 deaths a year, from veterans in wheelchairs to premature babies requiring life-support devices in the Neonatal Intensive Care Unit. Even physicians wearing respirator masks for hours can be prone to PIs.
Another complication of PIs is that no one knows exactly how long it takes for them to form. Currently, the only way medical staff can prevent PIs is by manually turning bedridden or critically ill patients every few hours.
One missed turn can lead to more medical complications. The U.S. spends nearly $27 billion annually on PI medical care. Given the country’s ongoing nursing shortage, a more automated PI monitoring method needs to be implemented. This could ensure that patients leave the hospital better than when they arrived.
To address this issue, researchers at Georgia Tech have developed a new, flexible, sensor-filled fabric to monitor areas at risk of PIs and alert hospital staff when a patient needs to be turned.
“I call this technology a paradigm shift,” said Sundaresan Jayaraman, a professor in the School of Materials Science and Engineering (MSE). “We’re using a fabric that acts like a bedsheet under the patient. It collects pressure and moisture data unobtrusively — whether you're lying in bed or sitting in a wheelchair. From this, we can predict when a PI is likely to occur and, more importantly, understand how long it takes to form.”
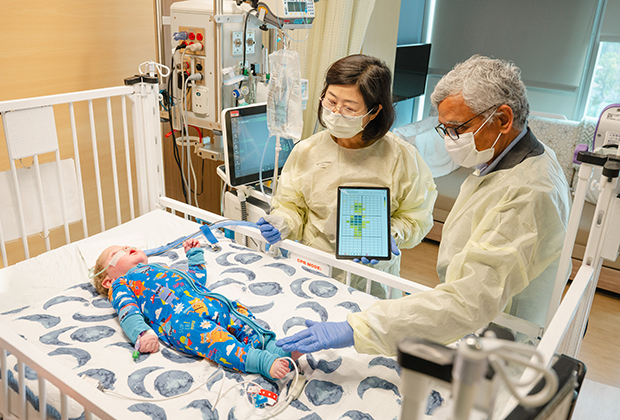
This technology is currently being piloted on four cribs in the Children’s Healthcare of Atlanta Arthur M. Blank Hospital Pediatric Intensive Care Unit (PICU), with the eventual goal of deploying it in 50 beds. The researchers hope their device becomes universal across healthcare systems, making PIs a thing of the past.